
Keratoconus is a progressive disease of the cornea that occurs in children, teenagers, and young adults. The cornea begins to thin causing the shape of the eye to change from a dome to a cone. The corneal curvature also becomes irregular. Before being diagnosed with Keratoconus, patients may begin to find that their glasses or contacts are no longer doing a good job correcting their vision or they may experience increasing unexplained astigmatism. Symptoms of Keratoconus may include blurred vision, difficulty seeing at night, light sensitivity, and halos and glare. Learn more about Keratoconus.
Dr. Herschel served as a Principal Investigator on an FDA multi-center Phase III clinical trial using corneal collagen cross-linking to treat patients with Keratoconus. The treatment was approved by the FDA in April 2016. Dr. Herschel was the only ophthalmologist in Central Florida participating in the trial, and our center has more experience treating patients with Keratoconus than any vision center in Central Florida. Meet Melanie, one of our cross-linking patients, and learn more about Dr. Herschel’s clinical trial experience.
Treatments for Keratoconus are intended to slow or stop the progression of the disease, stabilize the cornea, improve the corneal curvature, slow or stop further deterioration in vision, and improve the ability of glasses or contacts to correct vision. Over a number of months following treatment, the shape of the cornea and, therefore, visual acuity, will continue to change. After treatment, patients may likely continue to need glasses or contact lenses to correct their vision.
Did your doctor tell you that your only option is a Corneal Transplant? Learn about new advancements in treatment options
Keratoconus treatments are most often done in combination to optimize therapy for the underlying eye disease and maximize vision improvement. After a comprehensive vision history and eye examination, Dr. Herschel will discuss which treatments would be best for you. The treatments include:
- Specialty Contact Lenses
- Corneal Collagen Cross-Linking
- Intacs® Corneal Implants
- Topography-Guided PRK
- Conductive Keratoplasty
Specialty Contact Lenses
(RGP, Scleral Hybrid, Custom Soft Contact Lenses)
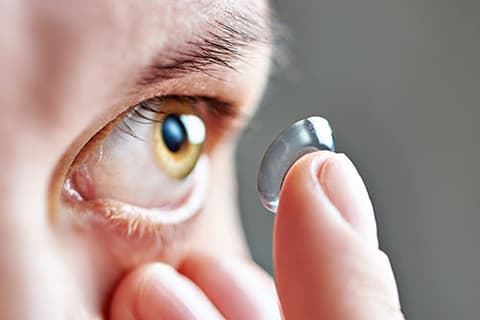
Modern contact lens designs for keratoconus are customized to the specific curvature of your eye. Many times, these lenses can improve vision, even in patients with more advanced disease.
Corneal Collagen Cross-Linking
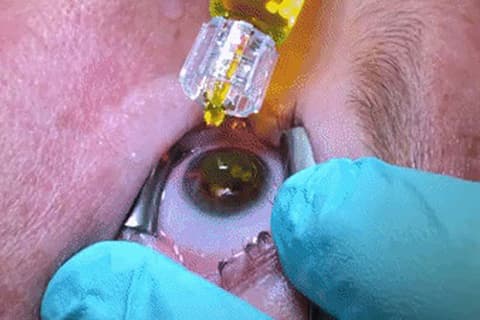
Corneal Collagen Cross-Linking is a procedure that uses riboflavin (Vitamin B2) in the presence of ultraviolet light (UV) to strengthen the collagen fibers in the cornea. This procedure slows or stops the progression of Keratoconus and helps improve the shape of the cornea and visual acuity (in most patients).
Intacs® Corneal Implants
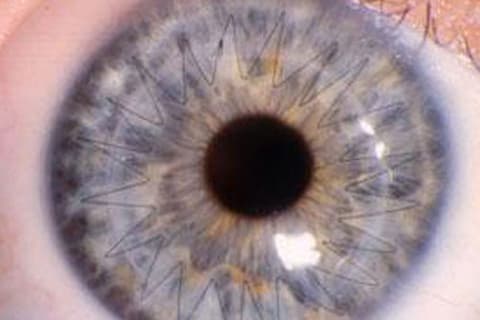
Intacs® Corneal Implants are thin, clear semi-circular plastic rings that are implanted in the eye with the goal of changing the shape of the cornea from the cone shape caused by Keratoconus towards the dome shape of the normal eye without removing any tissue from the cornea. The implants are intended to be permanent, but they can be removed, if vision needs change. The implants require no maintenance and cannot be felt. They are typically not visible to the naked eye.
Topography-Guided PRK

Topography-guided PRK uses topographic measurements to map the irregularities of a patient’s corneas and combines that information with refractive errors to produce a personalized treatment plan. This technology is well-suited for treating Keratoconus patients because Keratoconus patients have irregular corneas. In addition, Keratoconus patients may benefit from some combination of topography-guided PRK, corneal collagen cross-linking, Intacs® Corneal Implants, and conductive keratoplasty. After a comprehensive vision history and eye exam, Dr. Herschel will discuss with you what the best options are for your eyes. Learn more about Topography-Guided PRK.
Conductive Keratoplasty (CK)
Conductive keratoplasty is a simple procedure in which high-frequency radio waves are applied to the surface of the cornea. The waves shrink the tissue in small areas, thereby reshaping the cornea.
Signs and Symptoms of Keratoconus
Signs and Symptoms usually appear in the late teens and early twenties.

Excessively
Rubbing Eyes

Mildly
Blurry Vision

Difficulty
Seeing at Night

Frequent Changes in Eyeglass Prescriptions

Frequent
Headaches

Vision that Cannot Be Corrected with Glasses
For Which Keratoconus Treatments Am I a Candidate?
Since Keratoconus is a progressive disease, early diagnosis and treatment are very important. Dr. Herschel will review your vision history and perform a comprehensive evaluation of your eyes. This information is essential to determine the stage of your Keratoconus and the best treatment options or combinations available for you. Dr. Herschel will discuss your options with you.




